The
prognostic power of circulating cardiac biomarkers, their utility, and pattern
of release in coronavirus disease 2019 (COVID-19) patients have not been
clearly defined.
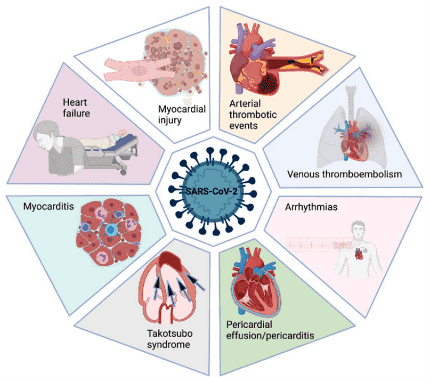
The
pandemic of coronavirus disease 2019 (COVID-19) caused by severe acute
respiratory syndrome coronavirus 2 (SARS-CoV-2) infection has led to over 474
million confirmed cases with 6,098,739 deaths worldwide by March 23rd, 2022.
Patients
with preexisting cardiovascular conditions are particularly at risk and have
poor prognoses. Clinical characteristics including heart rate, breath rate,
fever, cough, and dyspnea at the time of admission were analyzed. Laboratory
measurements including neutrophil count, CRP (C-reactive protein), cardiac
biomarkers (hs-cTnI, CK-MB, NT-proBNP [N-terminal proB-type natriuretic
peptide] or BNP [brain natriuretic peptide], MYO [myoglobin], and CK), and
inflammatory cytokine IL (interleukin)-6 at admission and during
hospitalization were extracted and analyzed.
Cardiac-specific
biomarkers, such as hs-cTnI, CK-MB, and (NT-pro)BNP. Compared with patients
without available myocardial biomarkers, patients with measured cardiac injury
markers had higher incidences of 28-day all-cause death and the occurrences of
Acute Respiratory Distress Syndrome, heart failure, disseminated intravascular
coagulation (DIC), sepsis, or multiorgan failure, and acute renal failure.
Prognostic
Performance of Cardiac Injury Biomarkers in Predicting 28-Day All-Cause
Mortality of COVID-19.
To
compare the relative accuracy, sensitivity, specificity, and positive and
negative predictive values of each biomarker based on laboratory defined ULN,
the prognostic performance of each marker was analyzed. The receiver operating
characteristic curve was used to demonstrate the ability of each cardiac
biomarker in discrimination of high risk of COVID-19 mortality, which was
quantitated as AUC.
Trajectory
Patterns of Cardiac Biomarkers and Inflammatory Factor Elevation in Patients
With COVID-19.
To
further demonstrate the mechanistic cause of cardiac injury in COVID-19
patients, Which determined the temporal relationship of cardiac biomarker
elevation with that of the inflammatory markers over time, it has been analyzed
the cumulative proportions of patients with increased cardiac biomarkers in
association with inflammatory factors of CRP, neutrophil count, and IL-6
elevation during the entire study period. This was based on the laboratory-defined
ULN and analyzed from the time of symptom onset (day 0) to the end of
follow-up.
In
patients showing heart injury during the entire hospitalization, neutrophil
percentage and CRP were rapidly and simultaneously increased after disease
onset, immediately by the increases of CK-MB, MYO, and hs-cTnI. In contrast,
the significant elevation of IL-6 occurred only after the increases of these
myocardial markers and was highly elevated mainly in patients with evidence of
cardiac injury. The increased inflammatory marker (CRP) and coagulation marker
(d-dimer) levels were also significantly associated with an increased risk of
28-day all-cause mortality of COVID-19 and had interactive effects with cardiac
injury markers in predicting the poor outcomes of COVID-19.
Elevations
of biomarkers such as hs-cTnI, CK-MB, (NT-pro)BNP, or MYO based on reference
laboratory normal cutoff values were highly prognostic of 28-day all-cause
mortality, including deaths occurring soon after admission. However, standard
cutoff values currently used for diagnosis likely underestimated the true
extent of cardiac injury. The newly established cutoffs in our study for
COVID-19 prognosis were much lower than the currently accepted laboratory
cutoff thresholds (by about 50%). The dynamic pattern of cardiac biomarker
elevation showed their onset coincided with CRP and neutrophil elevation but
preceded the elevation of IL-6.
The
company Biotime Biotechnology is a well-known POCT manufacturer that has
advanced cardiac markers which are used in the diagnosis and risk
stratification of patients with chest pain, suspected Acute Coronary
Syndrome(ACS), and Heart Failure(HF). Especially, 5 In 1 biomarker which
included 5 items on one cartridge (CTnI/ CK-MB/ Myo/ NT-ProBNP/ D-Dimer),
provides results within 15 minutes, has a wide detection range that can
accurately verify serious diseases, and is a convenience test with whole blood
or plasma without centrifugation. To properly evaluate patients with COVID-19
at admission, the cutoff threshold of abnormality for hs-cTnI, CK-MB, (NT-pro)
BNP, and MYO at admission should be lower than the currently recommended
laboratory range. Using standard reference laboratory cutoffs might
underestimate the extent of cardiac injury. Measurement of cardiac-specific
biomarkers like 5 In 1 (CTnI/ CK-MB/ Myo/ NT-ProBNP/ D-Dimer) Rapid
Quantitative Test at Biotime and proper interpretation on admission can help to
identify COVID-19 patients with a high-risk trajectory. The elevations can help
to provide references for the management, monitoring, and enrollment for
prospective studies and randomized controlled clinical trials.
In
conclusion, the abnormal cardiac biomarker pattern in COVID-19 patients was
significantly associated with increased mortality risk, and the newly
established COVID-19 prognostic cutoff values of hs-cTnI, CK-MB, (NT-pro)BNP,
CK, and MYO were found to be much lower (≈50%) than reference upper normal
limits for the general population. It is clinically meaningful that the fluctuating
levels of myocardial biomarkers should be intensively monitored, and patients
with elevated levels of those biomarkers should be intervened timely to improve
the prognosis of COVID-19. Our findings support additional prospective studies
and randomized controlled clinical trials to accurately validate the risk
thresholds and exact impact of myocardial injury for individuals with COVID-19.
Reference
1. World Health Organization.
Coronavirus disease (COVID-2019) situation reports. Coronavirus
Disease (COVID-2019) Situation Reports.
2020;2020. World Health Organization, Geneva.
2.
Liu PP, Blet A, Smyth D, Li H. The science underlying COVID-19: implications
for the cardiovascular system. Circulation. 2020;142:68–78. DOI: 10.1161/CIRCULATIONAHA.120.047549
3. Wu
F, Zhao S, Yu B, Chen Y-M, Wang W, Song Z-G, Hu Y, Tao Z-W,Tian J-H, Pei Y-Y,
et al. A new coronavirus
associated with human respiratory disease in China. Nature.
2020;579:265–269. doi: 10.1038/s41586-
020-2008-3
4.
Akhmerov A, Marbán E. COVID-19, and the heart. Circ Res.2020;126:1443–1455.
DOI: 10.1161/CIRCRESAHA.120.3170555. Gallagher PE, Ferrario CM, Tallant EA.
Regulation of ACE2 in cardiac myocytes and fibroblasts. Am J
Physiol Heart Circ Physiol.2008;295:H2373–H2379. DOI:
10.1152/ajpheart.00426.2008
5.
Shi S, Qin M, Shen B, Cai Y, Liu T, Yang F, Gong W, Liu X, Liang J, Zhao Q, et
al. Association of cardiac injury with mortality in hospitalized patients with
COVID-19 in Wuhan, China. JAMA Cardiol.
2020;5:802-810. DOI: 10.1001/jamacardio.2020.0950
6.
Guo T, Fan Y, Chen M, Wu X, Zhang L, He T, Wang H, Wan J, Wang X, Lu Z. Cardiovascular
implications of fatal outcomes of patients with coronavirus disease 2019
(COVID-19). JAMA Cardiol. 2020;5:1-8.
doi:10.1001/jamacardio.2020.1017
7.
World Health Organization. Laboratory Testing for 2019 Novel
Coronavirus (2019-nCoV) in Suspected Human Cases Interim Guidance. 2020. World Health Organization, Geneva.
8.
National Health Commission of China. New Coronavirus Pneumonia Prevention
and Control Program. 2020. National Health Commission of China. Beijing, China.
9. Zheng YY, Ma YT, Zhang JY, Xie X. Reply to: ‘interaction between RAAS inhibitors and ACE2 in the context of COVID-19’. Nat Rev Cardiol. 2020;17:313–314. DOI: 10.1038/s41569-020-0369-9